Statin Intolerance: What Are Your Options?
Struggling with statin side effects? Learn what statin intolerance really means, why it happens, and the evidence-based options available to safely lower your cardiovascular risk.
Dr Zohaib Iqbal
4/1/20264 min read

Statins are one of the most effective treatments available for reducing the risk of heart attack and stroke. They lower LDL cholesterol and, more importantly, reduce the number of atherogenic lipoprotein particles that drive atherosclerosis over time.
For most people, statins are safe, well tolerated, and life-saving. However, some individuals experience side effects — most commonly muscle-related symptoms — leading to what is often described as statin intolerance.
This is a common and important clinical issue, but it is often misunderstood. The key question is not simply whether symptoms occur, but whether they are truly caused by the statin, and how best to manage them without compromising long-term cardiovascular risk.
What is statin intolerance?
Statin intolerance refers to the inability to tolerate a statin at a dose required to adequately reduce cardiovascular risk due to side effects.
The most commonly reported symptoms include muscle aches, stiffness, fatigue, or weakness. Severe muscle injury is rare. In most cases, symptoms are mild and non-specific, and may not be directly caused by the medication itself.
Importantly, many patients who believe they are statin intolerant can, with the right approach, successfully take statin therapy.
Why do statin side effects occur?
There is no single explanation, and in many cases the cause is multifactorial.
Some individuals do experience genuine statin-related muscle symptoms. This may relate to how the drug is metabolised, interactions with other medications, or underlying factors such as thyroid dysfunction, vitamin D deficiency, or broader metabolic health.
However, muscle symptoms are also common in the general population. Large clinical trials have shown that similar symptoms occur at comparable rates in people taking statins and those taking placebo. This highlights an important point — not all symptoms that occur while taking a statin are necessarily caused by it.
There is also a recognised nocebo effect, where the expectation of side effects can contribute to symptom development. These symptoms are entirely real, but are not always directly driven by the medication itself.
Co-enzyme Q10 is sometimes discussed in this context. Statins can reduce circulating levels of co-enzyme Q10, which plays a role in cellular energy production, and this has led to the suggestion that supplementation may help reduce muscle symptoms. However, clinical evidence supporting its routine use is limited and inconsistent. While some individuals report benefit, it is not recommended as standard treatment in UK guidance, and in practice a structured approach to adjusting statin therapy or using alternative lipid-lowering strategies is usually more effective.
Why stopping statins matters
Stopping statin therapy without a clear plan can significantly increase long-term cardiovascular risk.
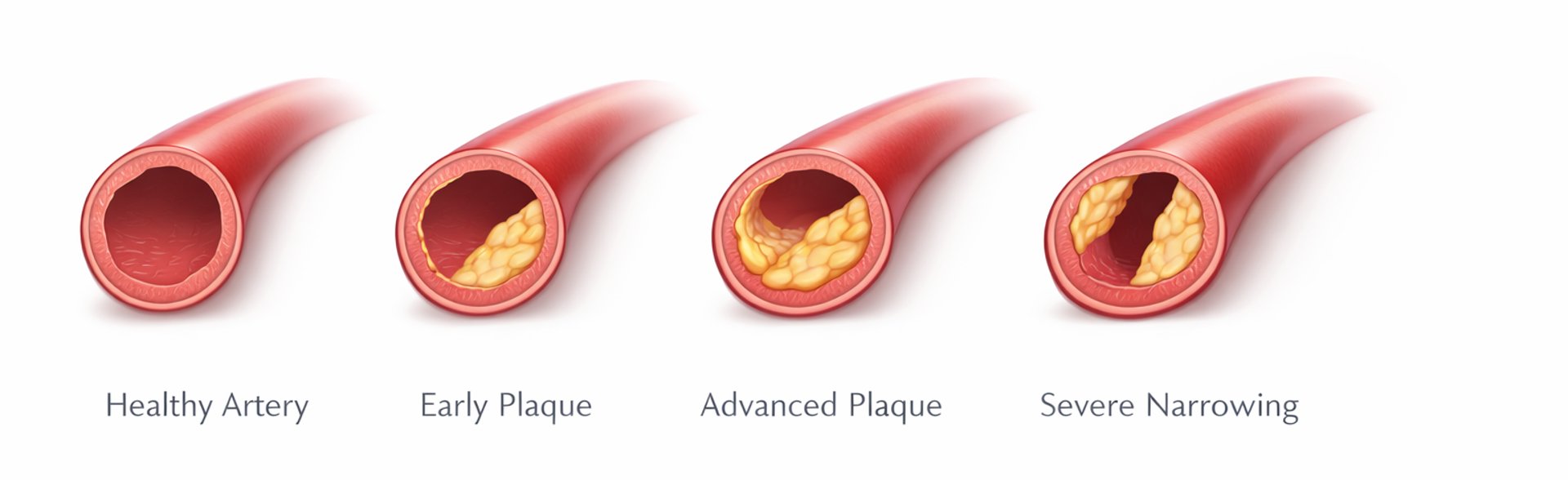
Atherosclerosis develops gradually over decades and is driven by cumulative exposure to atherogenic lipoproteins. Even modestly elevated cholesterol levels, when sustained over time, increase the likelihood of heart attack and stroke.
Evidence from large real-world studies has shown that discontinuing long-term statin therapy is associated with a higher risk of cardiovascular events, including heart attack and stroke, compared with continuing treatment.
For this reason, the goal is almost never simply to stop treatment, but to find an approach that is both effective and tolerable.
A structured, evidence-based approach
In the UK, the management of statin intolerance follows a clear framework aligned with NHS England guidance.
The NHS statin intolerance pathway outlines a systematic approach to assessment and management, emphasising:
Careful evaluation of symptoms and timing
Exclusion of alternative causes (e.g. thyroid dysfunction, vitamin D deficiency)
A “stop–rechallenge” strategy to confirm true intolerance
Avoiding premature discontinuation of therapy
This structured approach ensures that patients are not unnecessarily labelled as statin intolerant and that opportunities to safely continue treatment are not missed.
What are your options if you cannot tolerate statins?
A range of evidence-based strategies are available, and in many cases a workable solution can be found.
1. Trying a different statin
Not all statins behave the same way. Differences in metabolism and tissue distribution mean that a statin that causes symptoms in one person may be well tolerated in another.
2. Lower or intermittent dosing
Even low doses of statins provide meaningful cardiovascular benefit. Some patients tolerate alternate-day or twice-weekly dosing, which can still significantly reduce risk.
3. Combination therapy
Ezetimibe reduces cholesterol absorption from the intestine and is generally very well tolerated. When combined with low-dose statins, it can achieve substantial lipid reduction.
4. Advanced lipid-lowering therapies
For higher-risk individuals or those with confirmed statin intolerance, newer therapies such as PCSK9 inhibitors or inclisiran offer powerful LDL and ApoB reduction and are increasingly used in clinical practice.
5. Treating the right target
A more nuanced approach focuses on ApoB or non-HDL cholesterol, which better reflect the number of atherogenic particles. This allows treatment to be tailored more precisely rather than relying solely on LDL cholesterol.
The importance of specialist assessment
Statin intolerance is rarely straightforward. It sits at the intersection of symptoms, perception, metabolic health, and cardiovascular risk.
In many cases, patients labelled as statin intolerant can tolerate therapy when it is approached differently. Where true intolerance exists, alternative strategies can be implemented effectively.
A specialist lipid assessment allows:
Clarification of whether symptoms are truly statin-related
Individualised treatment planning
Access to advanced lipid testing (such as ApoB and lipoprotein(a))
Consideration of newer therapies where appropriate
When should you seek further advice?
You may benefit from specialist input if:
You have stopped statins due to side effects
You have tried multiple statins without success
Your cholesterol remains elevated despite treatment
You have a strong family history of heart disease
Your cardiovascular risk appears disproportionate to your cholesterol levels
Final thoughts
Experiencing side effects with statins can be frustrating, but it should not mean accepting untreated cardiovascular risk.
In most cases, there are multiple options available — and with the right approach, a safe and effective strategy can be found.
If you are unsure whether you are truly statin intolerant, or if your cholesterol remains difficult to manage, a more detailed and specialist-led assessment can help provide clarity and direction.
Contact
GMC Registered | NHS Consultant Endocrinologist
For Patients
© 2026. All rights reserved.
For Healthcare Professionals
Book a Consultation
Refer a Patient
